Ovarian cancer

Summary/Epidemiology
Ovarian cancer is a rare cancer. There are approximately 800 new cases per year in Belgium.
Risk factors
Most cases of ovarian cancer occur in women with no particular medical history, at menopause or beyond. There are genetic mutations that promote ovarian cancer and breast cancer. The responsible genes are called BRCA1 and BRCA2. In case of inactivating mutations in these genes, there is an increased risk of ovarian and breast cancer, often at earlier ages (on average 10 years). Mutations in these genes are passed from mothers to daughters as well as from fathers to daughters (i.e., not related to gender) and in families where these genes are mutated, there is usually a substantial number of breast and ovarian cancers in each generation. Due to the rarity of ovarian cancer, nowadays, each ovarian cancer patient is systematically seen by the oncogeneticist and a search for a mutation in these genes is performed. In suggestive families, an oncogenetic consultation is also planned to evaluate the need to perform the test (mutation risk score calculated). If a mutation is detected in a family member, the rest of the family, especially women, can be screened. In the event of a mutation being detected in a patient who is not yet affected by a cancer, special breast surveillance is offered and preventive removal of the ovaries between the ages of 35 and 45 is proposed, once the family planning has been completed.
Finally, in patients with ovarian cancer whose genetic tests have not shown a mutation in the BRCA1 and BRAC2 genes, a search for mutations in the tumor itself is also carried out, in order to be able to adapt the treatment with new therapeutic agents (see below).
Diagnosis
Ovarian cancer is difficult to diagnose because there are few or no specific symptoms of the disease.
Screening
Currently, there is no effective screening for ovarian cancer. Numerous large clinical studies have tried to find an effective screening, but all are negative so far. Diagnosing ovarian cancer at an early stage is not easy. Indeed, as the ovary does not have a capsule ("wrapping"), small clusters of cancerous cells, present on the surface of the ovary, quickly fall into the peritoneum (large membrane in which are contained all the organs of the abdomen, from the liver and diaphragm to the uterus, and containing the intestines, the spleen, the pancreas, etc.). These cells are carried away by the fluid that circulates continuously in the peritoneum and can then be deposited as small "candle spots" on the peritoneum, called peritoneal carcinomatosis. The latter reacts by producing fluid called ascites, which then accumulates in abnormal quantities in the abdomen. This condition can result in abdominal pain, discomfort and/or swelling. There is not always a clear image of the ovaries because small tumors can quickly lead to carcinomatosis.
Examinations
Confirmation of the diagnosis requires a biopsy performed during a "laparoscopy" or "coelioscopy". This minimally invasive technique allows visualization of the inside of the abdomen and the taking of samples or surgical treatment without opening the abdominal wall. It also allows to assess the importance of the tumor nodules implanted on the peritoneum and their extension on the abdominal organs, and thus to evaluate the best therapeutic strategy.
Treatments
Treatment of ovarian cancer is usually based on a combination of surgery, which must be radical, and chemotherapy.
Surgery
Surgery for ovarian cancer has made huge advances over the past two decades and is now considered the cornerstone of treatment. Indeed, pioneering European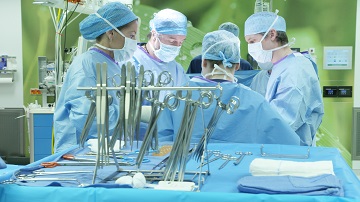 (Querleu et al., Dubois et al., etc.) and American (Chi et al., Bristow et al., etc.) teams have been able to demonstrate that the less residue left by surgery (i.e. disease at the end of the surgery), the better the outcome for the patients, in terms of number of recurrences and response to treatment at the time of the recurrences, and therefore survival rate.
(Querleu et al., Dubois et al., etc.) and American (Chi et al., Bristow et al., etc.) teams have been able to demonstrate that the less residue left by surgery (i.e. disease at the end of the surgery), the better the outcome for the patients, in terms of number of recurrences and response to treatment at the time of the recurrences, and therefore survival rate.
In practice, ovarian cancer surgery, namely peritoneal surgery (given the development of the disease mainly in the peritoneum), requires special training; all the onco-gynecologic surgeons of the Cliniques Universitaires Saint-Luc and associated network have been trained in this particular surgery, for the most part in France, where the techniques have been developed for many years. This surgery also sometimes entails extensive visceral procedures, where the assistance of a colorectal or hepatobiliary surgeon may be required. The oncological expertise of the King Albert II Institute surgeons in the treatment of cancer and the way of working within the university clinics allow an easy collaboration and guarantee an optimal quality of all the procedures carried out, each of the operators being at the forefront of their discipline..
Chemotherapy
Chemotherapy for ovarian cancer usually combines two molecules, carboplatin and paclitaxel, in 6 courses once every three weeks. This combination is very effective in the treatment of ovarian cancer and is administered either as an adjuvant treatment, i.e. after surgery, or as a neoadjuvant treatment, i.e. before surgery when the latter seems too extensive or impossible to perform with zero residue based on the initial laparoscopy performed (see above). The available literature data do not show any difference between the two strategies in terms of recurrence and survival. In the neoadjuvant setting, 3 courses are given before surgery and 3 after..
In addition to conventional chemotherapy, new molecules called targeted therapies have emerged in the treatment of cancer in recent years:
• Bevacizumab: This is an antibody directed against molecules that stimulate the growth of blood vessels to the tumor. This prevents the tumor from forming new blood vessels, which are necessary to provide oxygen and nutrients for the tumor to grow. This agent has shown good efficacy, particularly in advanced stages and in cases of rapid recurrence after the first treatments. It is administered by infusion once every three weeks and is reimbursed in Belgium for certain indications. There are very few adverse effects that are closely monitored during treatment.
• PARP inhibitors: DNA repair pathways are essential for tumor cells. BRCA1 and BRCA2 proteins play a crucial role in the homologous recombination (HR) DNA repair pathway. This DNA repair pathway is impaired when BRCA1 or BRCA2 is inactivated, which is systematically the case in tumor cells of patients with a constitutional, i.e. inherited, mutation in the BRCA1 or BRCA2 genes. However, this can also occur in tumor cells from patients who do not have an inherited predisposition to breast or ovarian cancer. This inactivation of BRCA1 or BRCA2, whatever the cause, renders the HR DNA repair pathway ineffective in tumor cells, but there is still the "base excision repair" (BER) pathway. When tumor cells are damaged by chemotherapy, they can still repair their DNA through this second pathway and thus resist to treatment. New treatments, PARP (poly-ADP-ribose-polymerase) inhibitors, inactivate this second DNA repair pathway. Three PARP inhibitors are currently available: olaparib, niraparib, and veliparib. Olaparib is presently reimbursed for mutated patients at the time of their first recurrence. They markedly increase the survival of these patients.
• Recently, the SOLO 1 study showed a high efficacy in BRCA mutated patients in the first line (i.e. just after the first treatment, in "maintenance"). In this study, more than half of the patients had not relapsed at 5 years after treatment, which is exceptional in this disease. Consequently, olaparib is now also reimbursed in these first-line patients.
• New targeted therapies are used in large international studies in which reference centers, such as the King Albert II Institute, take an active part. Our patients can therefore benefit from innovative treatments that are not yet available on the market, free of charge, within the framework of these studies.
• Finally, immunotherapy, which is very effective in some cancers, has shown disappointing results in ovarian cancer, and basic research in immunology is one of the major activities in our group (2 academic research projects in progress, a doctoral thesis in progress) in order to try to understand why and to improve the effectiveness of these treatments.
Conclusion:
Optimal treatment requires a multidisciplinary and centralized approach. The frequent combination of the different therapeutic options of surgery, radiation therapy, and chemotherapy illustrates the need to correctly define the characteristics of the cancer. This approach makes it possible to establish the care plan and the sequence of treatments. This requires the cooperation of specialists in imaging or microscopy capable of assessing the aggressiveness of the cancer and its extent.
The weekly multidisciplinary meetings organized at the King Albert II Institute therefore include all the specialists involved in the diagnosis and treatment of gynecological tumors. They make it possible to identify the most appropriate therapeutic attitude for each patient, in accordance with current standards of care.
Fertility preservation and cancer treatments
Cancer treatments, regardless of the location of the tumor, are sometimes detrimental to women's fertility. Ovarian tissue cryopreservation or oocyte cryopreservation (depending on the situation and the time available) carried out at the King Albert II Institute allows to overcome this inconvenience. It consists in retrieving a fragment of ovary or directly the oocytes from the ovaries after ovarian stimulation (oocyte cryopreservation) and to freeze them before starting the cancer treatment potentially harmful to fertility. At the end of the treatment, the ovarian fragment is re-implanted by laparoscopy or the oocytes are used for in vitro fertilization. These techniques are now being reimbursed since June 2017 in the context of cancer. To learn more about this technique, click here.
Research / Innovation
A multicenter observational study is currently being conducted in several centers in Belgium, initiated by the King Albert II Institute onco-pelvi group, of which they are the principal investigators.
European accreditation
In 2016, the European Society of Gynaecological Oncology (ESGO) published quality criteria for ovarian cancer surgery.
The first criterion, which is necessary to apply for European accreditation, is the number of cases operated on per year (minimum 20 cases/year). In Belgium, most patients with ovarian cancer are treated in centers that operate on less than 5 cases per year. In order to achieve this quantitative objective, to improve the quality of care at the King Albert II Institute and at the same time to allow the collaborating center to treat patients within their hospital, a network of gynecological oncology was created within the King Albert II Institute at the initiative of the onco-gyneco group of the Cliniques Universitaires Saint-Luc (Dr Luyckx, Prof Squifflet, Prof Baurain). The UNGO (UCL Network of Gynaecological Oncology) was born in 2016. In practice, patients diagnosed with ovarian cancer in one of the network centers are discussed at the local multidisciplinary oncology consultation (MOC) and then at the one in Saint-Luc in order to determine the treatment plan. Chemotherapy (see below), all examinations, and follow-ups are carried out at the initial site, but surgery is performed at the Cliniques Universitaires Saint-Luc by a multidisciplinary surgical team under the supervision of gynecological oncologists: one of the two onco-gynecologists at Saint-Luc (Prof Squifflet, Dr Luyckx) and the gynecological oncologist at the referral site, appointed as an external consultant in the gynecological department of the Cliniques Universitaires Saint-Luc. Post-operative care is provided at the Cliniques Universitaires Saint-Luc, after which the patient is readmitted to the initial center for further treatment and follow-up.
The centers composing this network of centralization of ovarian cancers at the Cliniques Universitaires Saint-Luc are:
- the hospital center of Picardy Wallonia (CHWaPi) in Tournai (Dr Jouret),
- the Europe hospitals in Brussels (Dr Grandjean for the St-Michel site and Dr Waterkeyn for the St-Elisabeth site),
- the Clinic Saint-Jean in Brussels (Dr Van Gossum).
In 2019, two additional centers joined the UNGO:
- the Clinic St-Pierre in Ottignies (Dr Malvaux and Dr Lousse)
- the CHC in Rocourt (Dr Tock).
In the first quarter of 2019, the Cliniques Universitaires Saint-Luc and UNGO received the ESGO accreditation for advanced ovarian cancer surgery.
Here is a video explaining how the UNGO and accreditation work.
Contact
For any further information, or if you would like to make an appointment, please contact the Oncology Care Coordinator at + 32 2 764 94 08.
Doctor

Pr Jean-Francois BAURAIN

Dr Frank CORNELIS

Dr Sophie CVILIC
Dr Latifa FELLAH
Quitteries FONTANGES
Dr Aline FRANCOIS

Dr Amandine GERDAY

Dr Pascale JADOUL

Dr Carine KIRKOVE

Dr Isabelle LECONTE

Dr Mathieu LUYCKX
Dr Charlotte MAILLARD

Dr Filomena MAZZEO

Dr Vasiliki PERLEPE

Pr Jean-Luc SQUIFFLET
Paramedical

Laurence BEAUSAERT
Ingrid DE BIOURGE

Fanny DEPRÉ

Maëlle DETRY

Naila EL IDRISSI

Louise FAVARETTO

Florence FONTAINE

Monique KASA VUBU

